When Shoulder Pain Limits How You Move and Function
Shoulder pain often affects more than one movement. Reaching overhead, lifting objects, sleeping, getting dressed, or exercising can become difficult or uncomfortable. Because the shoulder is involved in so many daily and recreational activities, pain in this area can quickly feel frustrating and limiting.
Shoulder pain is a common experience among patients, and whether it’s tendinitis, a tear, or some other factor, there could be numerous reasons for the pain you’re feeling. Many people seek shoulder pain relief in Illinois when discomfort begins to interfere with work, fitness routines, or everyday tasks. At IMPACT Physical Therapy & Sports Recovery, physical therapy and athletic training helps people regain strength, mobility, and confidence in shoulder movement.
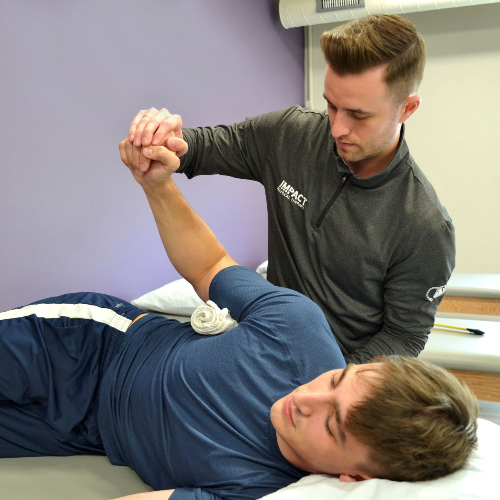
Common Shoulder Pain Conditions
Post-Surgical
There are a variety of shoulder surgeries that may have to be done in order to stabilize the shoulder, repair damaged tendons or ligaments. With the advances in arthroscopic surgery, recovery times for shoulder injuries have improved, however physical therapy is still needed to reduce pain quickly, restore range of motion, improve strength and return the individual to the normal activities they like to do.
Sprain / Strain
A sprain in the shoulder involves the ligaments while a strain involves the muscles around the shoulder. A sprain / strain typically occurs because the tissue has been overstretched too quickly, resulting in micro-tearing of the tissue. This results in painful inflammation, typically increased with movement and use of the damaged tissue.
The damage from a sprain / strain can be minor or major, depending on the severity of the injury, person’s health and age. As we age, our tissue becomes less elastic and becomes more prone to tearing.
Frozen Shoulder
Frozen shoulder is a painful shoulder joint condition. In medical terminology it is called “adhesive capsulitis”. How frozen shoulder exactly begins is still a bit of a mystery, however, it typically occurs after a trauma or repetitive injury to the shoulder. Women in the pre and post–menopausal age range are more likely to experience frozen shoulder, however men can also experience frozen shoulder.
With frozen shoulder, the thick capsule of tissue that surrounds the shoulder joint begins to experience chronic inflammation. The body begins a cycle of inflammation and scarring that causes the capsule around the shoulder joint to contract and become limited in its flexibility. This causes very painful range of motion in the shoulder when trying to move the arm.
At the beginning of frozen shoulder it is very painful and range of motion becomes limited. This can be around 4–8 weeks in duration. After that, motion is very limited in the shoulder, but often not as painful. Depending on the severity of the condition, it can take sometimes up to a year to resolve and improve range of motion.
Dislocation
Dislocation of the shoulder typically occurs from falling onto an outstretched arm or a blow to the side or back of the shoulder when falling on it. This can happen in different sports activities or falls. Dislocations are managed medically to relocate the head of the humerus bone. Depending on the severity of the dislocation, your physician will typically prescribe physical therapy to help stabilize the shoulder joint and protect it during a recovery phase.
With frequent dislocations, the shoulder can become unstable as many structures in the shoulder get damaged and become too lax. By strengthening the muscles around the shoulder, stability can be increased in the shoulder, preventing future dislocations.
At times, dislocations can be quite severe and lead to tearing of cartilage, tendons, ligaments or muscles. In this case, surgery is often needed. After surgery physical therapy is an important part of recovery and returning to normal activities.
Labrum Tear
The labrum is a thick ring of cartilage around the socket part of your shoulder joint (glenohumeral joint). The labrum acts like a cup for the head of the humerus to sit in (like a ball inside a cup). The labrum gives stability to the joint and also helps to cushion as the shoulder joint moves.
The labrum can tear with injury from a blow to an outstretched arm or from repetitive injuries overhead. Sometimes, a labrum tear can be involved when the rotator cuff is torn. A common tear is called a SLAP lesion (Superior Labral tear from Anterior to Posterior). This is a tear of the labrum from the top part in front to back. This often needs surgical repair and we work with your physician on their protocol to rehab your shoulder after surgery.
Rotator Cuff
The rotator cuff is a group of muscles surrounding the shoulder. They are made up of the supraspinatus, infraspinatus, sub–scapularis and teres minor muscles. While these muscles are small and not that powerful, they play a critical role in how the shoulder moves. Without your rotator cuff, you would not be able to lift your arm very far from your side. The job of the rotator cuff is to guide the direction of the humerus head down and spin so that it clears the bony shelf above the socket called the acromion. When the rotator cuff is weak, the head of the humerus rides up slamming into the acromion above it.
The rotator cuff takes a lot of abuse over a lifetime and tearing is very common as we age. Many factors can lead to injury to the rotator cuff such as sports injuries, falls onto the shoulder or arm, repeat lifting or movements, poor posture or heavy lifting in abnormal positions.
Rotator cuff tears can be minor, causing pain and inflammation, or major which can require surgery. With surgery, depending on a variety factors such as the quality of the tissue, the extent of the tear and other health factors, the recovery can take between 3-6 months. Physical therapy is a very important part of preparing for surgery and rehabilitating after surgery.
Sports Injuries
Whether you are a professional athlete, high school athlete or just like to be active and play sports, injuries can occur. Many shoulder sports injuries occur because of a fall onto an outstretched arm or from repetitive overhead actions, such as swimming or tennis. Another reason for shoulder sports injuries is an imbalance which can occur in certain groups of the shoulder muscles if one group of muscles is stronger than another. For example, an athlete that has strong chest muscles, but weak rotator cuff muscles can put themselves at risk of injury.
Bursitis / Tendonitis
The ending of the word “itis” is defined as inflammation. Therefore, bursitis is inflammation of a bursa and tendonitis is inflammation of a tendon. A bursa is a fluid filled sac that sits between muscles or tissues to cushion and reduce friction. In the shoulder there is a rather large bursa between the deltoid muscle and joint. This is called the sub-deltoid bursa. This bursa can often become inflamed due to abnormal joint movements, poor posture and weakness of the surrounding musculature. This causes strain to the tissues and excessive friction on the bursa. People tend to feel pain with movement and especially movement out to the side or reaching behind them.
Tendons connect muscles to bones. In the shoulder common areas for tendonitis are in the rotator cuff tendons (supraspinatus, infraspinatus, teres minor and subscapularis) and bicep tendons. Pain can be felt deep in the shoulder or in the front of the shoulder. Pain is usually felt as a sharp, catching sensation with certain movements.
Why Shoulder Pain Develops and Why Addressing It Matters
The shoulder joint relies on coordinated movement between muscles, tendons, and joints. Pain can develop gradually from overuse or appear suddenly after an injury or increase in activity.
Shoulder pain may be caused by injury, overuse, muscle strain, joint irritation, or wear and tear over time. Common conditions include rotator cuff irritation, tendon inflammation, joint stiffness, and instability. Without proper care, shoulder pain can lead to compensatory movement patterns that place added stress on surrounding structures.
Timely physical therapy supports function by improving movement quality, restoring strength, and helping people continue daily activities with less discomfort.
Common Symptoms That Affect Shoulder Function
People experiencing shoulder pain may notice:
- Pain with reaching or lifting
- Difficulty raising their arm overhead
- Weakness in the shoulder or upper arm
- Stiffness that limits range of motion
- Pain that worsens with activity
- Discomfort when sleeping on the affected side
- Clicking or catching sensations with movement
- Reduced tolerance for work or exercise
Symptoms may vary based on the cause of shoulder pain and the activities that aggravate it.
How Care Is Provided at IMPACT Physical Therapy & Sports Recovery
Physical therapy at IMPACT Physical Therapy & Sports Recovery focuses on understanding how shoulder pain affects daily movement. Care begins with a detailed evaluation of shoulder mobility, strength, posture, and movement patterns.
Treatment methods commonly used for shoulder pain include:
- Manual therapy, used to improve joint and soft tissue mobility and reduce stiffness
- Graston Techniques, applied to address soft tissue restriction and support smoother movement
- ASTYM® Therapy, used to help stimulate the body’s natural healing response and improve tissue tolerance
- Trigger point dry needling, when muscle tension contributes to pain or restricted motion
- Therapeutic exercise, focused on strengthening the rotator cuff and surrounding muscles to improve stability
- Movement retraining, helping correct patterns that place excess stress on the shoulder
- Athletic training principles, when appropriate, to support return to sport, lifting, or overhead activity
Each approach is selected based on how symptoms present and what the patient wants to return to.
Care That Reflects Skill, Attention, and Purpose
At IMPACT Physical Therapy & Sports Recovery, we’re proud to offer personalized, one-on-one care in a warm and welcoming environment. As a physical therapist-owned practice, the team values hands-on treatment, clear communication, and thoughtful progression.
We’ve grown with one purpose in mind: helping people get back to doing what they love using highly skilled manual techniques. This commitment guides how shoulder pain is treated across Illinois.
Take the Next Step Toward Comfortable Shoulder Movement
If shoulder pain is limiting your ability to work, stay active, or enjoy daily life, contact IMPACT Physical Therapy & Sports Recovery to request an appointment and learn how individualized physical therapy and athletic training can help you regain strength, mobility, and confidence.
Frequently Asked Questions About Shoulder Pain
What types of shoulder conditions can physical therapy help?
Can physical therapy help shoulder pain without surgery?
How long does it take to see improvement in shoulder pain?
We provide shoulder pain relief in all of our clinics: Champaign, IL, Hinsdale, IL, Lakeview in Chicago, IL, Naperville, IL, Norridge in Chicago, IL, Oak Lawn, IL, Orland-Park, IL and South-Loop in Chicago, IL

