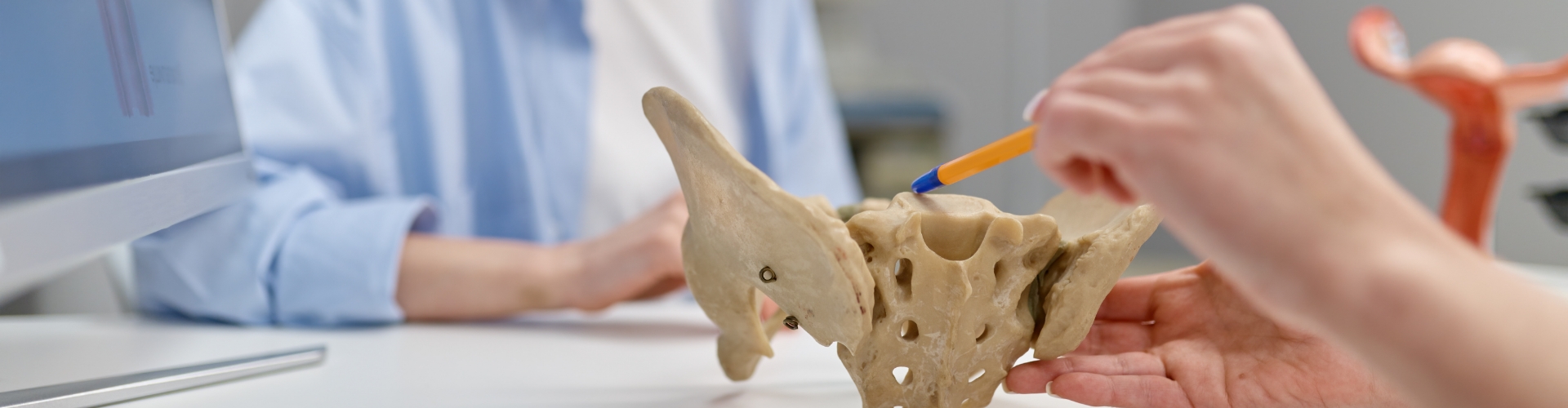
When Pelvic Floor Symptoms Disrupt Daily Life
Pelvic floor dysfunction can affect comfort, confidence, and everyday routines. Sitting, walking, exercising, using the bathroom, or engaging in intimacy may feel uncomfortable or difficult. Many people experience frustration when symptoms interfere with activities they once did without thinking.
The pelvic -floor muscles help control urine flow, support pelvic organs, stabilize the low back, and aid in sexual function. When these muscles are not working properly, symptoms can appear in different ways. At IMPACT Physical Therapy & Sports Recovery, physical therapy helps people suffering with pelvic floor dysfunction in Illinois so daily life feels more manageable and comfortable again.

Why Pelvic Floor Dysfunction Occurs and Why Care Matters
Pelvic floor dysfunction can develop for many reasons. Changes in muscle strength, coordination, or tissue mobility can affect how the pelvic floor supports the body.
Pelvic pain is pain felt in the lower abdomen, pelvis, or perineum, and may be linked to muscle weakness or imbalance within the pelvic floor, trunk, or pelvis. Pregnancy, childbirth, surgery, scar tissue, nerve pressure, and repetitive strain can all contribute to symptoms. Pelvic floor dysfunction can affect people of all genders and ages.
Addressing symptoms early helps restore function, improve comfort, and support confidence with daily activities, without relying solely on medication or invasive procedures.
Common Symptoms of Pelvic Floor Dysfunction
People with pelvic floor dysfunction may experience:
- Urinary leakage or urgency
- Pelvic or lower abdominal pain
- Difficulty with bowel movements
- Pain during sexual activity
- A feeling of heaviness or pressure
- Tailbone, hip, or pubic bone pain
- Difficulty sitting or standing comfortably
- Reduced core stability
Symptoms vary based on which muscles, nerves, or tissues are involved.
How Pelvic Health Care Is Provided at IMPACT Physical Therapy & Sports Recovery
Pelvic floor physical therapy at IMPACT Physical Therapy & Sports Recovery begins with a thorough evaluation to understand how symptoms affect daily life. Pelvic health specialists assess posture, movement, breathing patterns, muscle coordination, and pelvic floor function.
Treatment approaches may include:
- Pelvic floor muscle training, improving strength and coordination to support bladder, bowel, and core control
- Manual therapy, addressing soft tissue restriction and tenderness within the pelvis
- Biofeedback, helping patients improve awareness and control of pelvic floor muscles
- Electrical stimulation, when appropriate, to assist muscle activation and coordination
- Movement and postural retraining, reducing strain during daily activities
- Athletic training principles, when appropriate, to support return to exercise and higher-level movement
Each plan is tailored to individual symptoms and goals.
Specific Pelvic Health Concerns We Can Help Address
Diastasis Recti
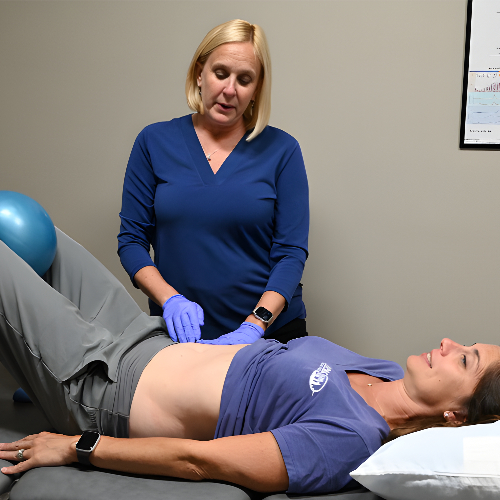
Diastasis recti refers to a separation of the abdominal muscles that often occurs during or after pregnancy, but it can also affect individuals outside of pregnancy. This separation can impact core strength, posture, and pelvic floor function. People with diastasis recti may notice abdominal doming, back discomfort, or difficulty engaging their core during movement.
At IMPACT Physical Therapy & Sports Recovery, physical therapy addresses diastasis recti by improving how the abdominal muscles, pelvic floor, and breathing system work together. Treatment focuses on restoring coordinated muscle activation rather than simply closing the gap. Guided exercises help rebuild functional core strength, support the low back, and improve stability during daily tasks such as lifting, bending, and carrying. This approach helps patients move with greater confidence and control.
Incontinence
Urinary incontinence is the involuntary leakage of urine, which can happen at any time. It may occur with coughing, sneezing, exercise, or strong urges to urinate. Incontinence is often related to weakness or dysfunction in the pelvic-floor muscles, which play a key role in bladder control.
The pelvic health team at IMPACT Physical Therapy & Sports Recovery specializes in treating urinary incontinence through personalized physical therapy. Care focuses on strengthening and coordinating the pelvic floor muscles, improving bladder habits, and reducing leakage episodes. Treatment plans are designed to help patients regain confidence and return to daily activities without constantly worrying about bathroom access. Physical therapy provides a conservative, effective option for managing incontinence and improving quality of life.

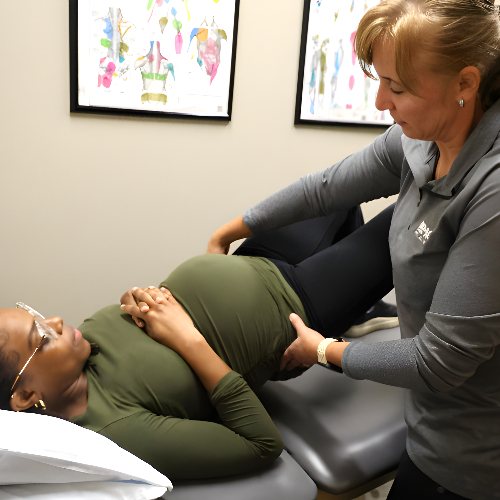
Prenatal & Postnatal Care
Pregnancy and childbirth place significant demands on the pelvic floor, abdominal muscles, and surrounding structures. Many individuals experience pelvic pain, incontinence, or core weakness during pregnancy or after delivery.
At IMPACT Physical Therapy & Sports Recovery, prenatal and postnatal physical therapy supports the body through these changes. Care focuses on maintaining strength, mobility, and comfort during pregnancy, while postnatal therapy helps restore pelvic floor and core function after childbirth. Treatment may address pelvic pain, scar tissue, muscle imbalance, and movement strategies for daily activities. This supportive approach helps individuals recover safely, reduce symptoms, and feel more confident as they return to regular activity and exercise.
Care Built on Skill and Personal Attention
We aim to create a place where expert care meets genuine passion, and where every patient receives personalized, one-on-one attention in a warm and welcoming setting. Pelvic health care at IMPACT Physical Therapy & Sports Recovery reflects this commitment through thoughtful, individualized treatment.
We’ve grown with one purpose in mind: helping people get back to doing what they love using highly skilled manual techniques. This philosophy guides pelvic floor care across Illinois.
Take the Next Step Toward Pelvic Health
If pelvic floor dysfunction is affecting your comfort, confidence, or daily life, contact IMPACT Physical Therapy & Sports Recovery to request an appointment and learn how personalized pelvic health physical therapy can support your recovery and long-term function.
Frequently Asked Questions About Pelvic Floor Dysfunction
Can pelvic floor physical therapy help with sexual dysfunction?
Is pelvic floor therapy only for women?
Can pelvic floor therapy help with bowel control issues?
We provide pelvic floor at the following locations: Champaign, IL, Hinsdale, IL, Lakeview, IL, Naperville, IL, Orland-Park, IL, South-Loop, IL