To understand the impacts of chronic pain, it is important first to recognize that each individual’s experience with pain is unique. A physical therapist’s role is to be an active listener and educator to work with the patient to navigate their pain story. Learn more about the process of chronic pain management and how this course of treatment can help you at IMPACT Physical Therapy.
Different Types of Pain
Before seeking physical therapy for chronic pain, it is important to understand pain and the differences between acute and chronic pain:
- Pain is a normal human experience; unpleasant sensory and emotional experiences associated with actual or potential tissue damage but may not involve actual tissue damage.
- Acute pain is an immediate response to an experience or noxious stimuli, typically shorter in duration.
- Chronic pain is a multi-component complex reality involving emotional, cognitive, neurological, social, and environmental factors.
Acute vs. Chronic Pain & Pain Response
Acute Pain
Acute pain becomes chronic pain when persisting even after tissue healing. An example to explain the pain response is stepping on a nail. In an individual not experiencing chronic pain, before making contact with the nail, the body has low pain input activity. Upon contact with the nail, the body’s alarm activates, sending signals to the brain exciting high pain activity resulting in pain perception. Pain activity remains high until the removal of painful stimuli – upon which pain activity returns to its baseline. In an individual experiencing chronic pain, pain activity remains high even after removing the painful stimuli.
Chronic Pain
Chronic pain develops from trauma, distress, fear-avoidance, personal beliefs, stress, and pain catastrophization. Unpacking the multiple factors that impact chronic pain is vital to addressing behavioral pain provocation. The pain cycle occurs when pain persists, spreads, and worsens, leading to painful movement, decreased pain predictability, reduced pain threshold, nociceptor hypersensitivity, and an increased link between pain and thoughts, feelings, and threats.
Pain Response
This response results in guarding, apprehension, and avoidance behaviors further feeding into:
- Wind-up: increased response to pain signals
- Allodynia: hypersensitivity to light touch, and excessive response to normally noxious stimuli
- Hyperalgesia: extreme response to normally noxious stimuli
The body remains in a heightened state of sensitivity with increased heart rate, alertness, use of energy stores, and inflammation.
Purpose of Pain
Pain is multifactorial and occurs throughout somatic, psychological, and social domains. Pain does not provide a measure of the state of tissue health or damage but correlates with bodily danger. The body’s alarm system activates to mitigate threats working similarly to that of a house. A house’s alarm system — in this example, the body — does not activate unless a window or door breaks signaling danger, which initiates a cascade of events to mitigate that danger. A house in a chronic pain state will have an over-sensitized alarm system that will activate when a car drives by or walks their dog on the sidewalk. This scenario is an example of allodynia, or when usually innocuous stimuli are now noxious.
Chronic Pain Management
Physical therapists have an important role in the healthcare team, providing collaborative care to treat chronic pain. A physical therapist offers compassion and empathy to an individual’s pain story. Chronic pain management includes providing education, explanations, guidance, and motivation. Creating an individualized plan to treat chronic pain with physical therapy includes graded exercise, aerobic capacity, and progressive exposure. A physical therapist assists with goal setting, sleep schedules, hygiene, and nutrition. They use a variety of interventions to treat chronic pain, some of which include:
- Soft tissue massage
- Joint and neural mobilization
- Trunk stabilization
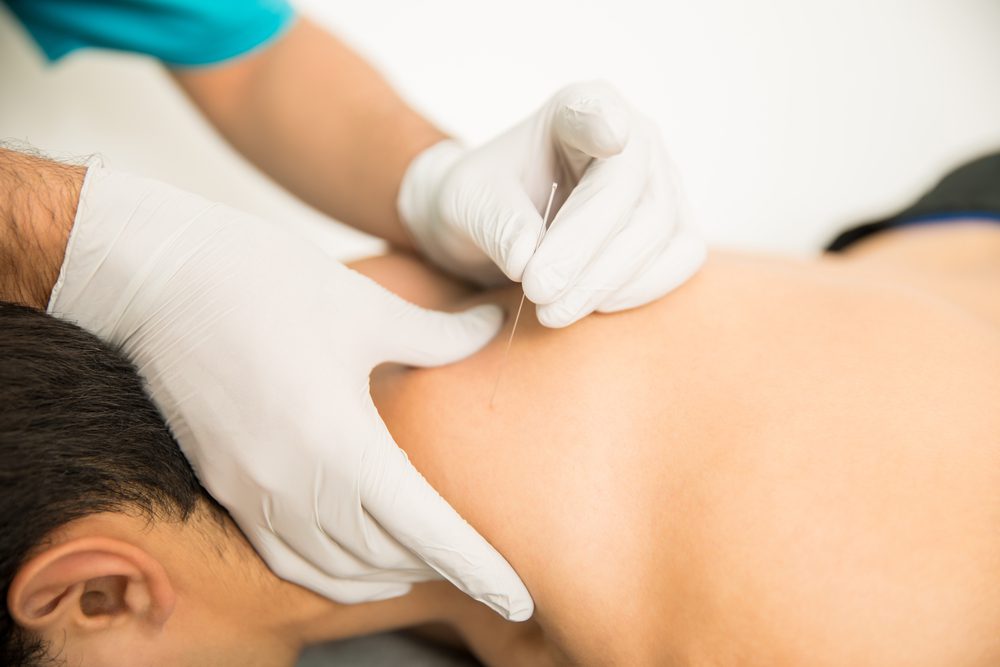
- Trigger point dry needling
- Modalities
- Breathing exercises
Treating the impact of chronic pain is not a quick fix and often requires activity modification, behavior management, multi-faceted care, and lifestyle changes. How one understands and copes with pain affects how one experiences it. It is important to understand that hurt does not equal harm, and the amount of pain perceived does not necessarily equate to the amount of tissue damage present. Being educated provides understanding and empowerment to be independent in pain management. Research supports receiving pain neuroscience education provides improved pain rating, pain knowledge, disability, pain catastrophization, fear-avoidance, physical movement, healthcare utilization, and attitudes and behaviors regarding pain. With the foundation of education, the next step is to move.
Movement Physical Therapy for Chronic Pain
Motion is lotion! Movement and activity are the most effective pain killers on the planet. A six-mile run stimulates endorphin release that is equivalent to ten milligrams of morphine. Exercise is vital for pain management. Physical therapists are movement specialists with expertise in choosing safe exercise, establishing a baseline, and creating a progression plan. Important principles to keep in mind when establishing and progressing a physical therapy for chronic pain movement program are:
- As you exercise, be patient, be persistent, and gradually increase your daily exercises.
- Flare-ups can occur, and when it happens, adjust programming and continue with gradual increases to limit recurrences.
- Exercise the mind by utilizing visualization to imagine performing activities to regulate the brain to perform tasks pain-free.
- Perform activities in various environments, introduce distractions, and move during different emotional states.
- Keep a log of progress to track goals and continue to plan exercise ahead of time so that the what, when, and how are written out.
- Find the balance between “no pain, no gain” and “if it hurts, don’t do it.”
- Focus on function and accomplishments to deter attention from pain perseveration.
Post-Exercise Recovery
An important aspect of exercise often overlooked is recovery, and one of the best recovery methods is getting consistent sleep. To maximize sleep and recovery, it is best to do the following:
- Maintain a consistent bedtime and wake-up time
- Eliminate naps during the day, or limit to 20 minutes maximum
- Attempt to stay in bed even if you cannot sleep
- Turn off electronics 1-2 hours before bed and avoid checking emails and messages
- Decrease fluid intake before bed as well as avoid alcoholic beverage and caffeine intake in the late afternoon or evening
- Remove pets and children from the bed
- Keep a sleep log to write down any lingering thoughts
- Utilize relaxation and meditation methods
- Exercise during the day
Find Help For Your Chronic Pain Today!
All pain is real, and the impacts of chronic pain are manageable with physical therapy. IMPACT Physical Therapy can assist with education, exercise, sleep, activity modification, and pain management. Contact a location near you to find a skilled physical therapist to help you with creating a plan for physical therapy for your chronic pain.